Normally, a pregnancy lasts for approximately 40 weeks. When a baby is born before completing 37 weeks of pregnancy, it is considered to be preterm.
There are three categories of preterm birth:
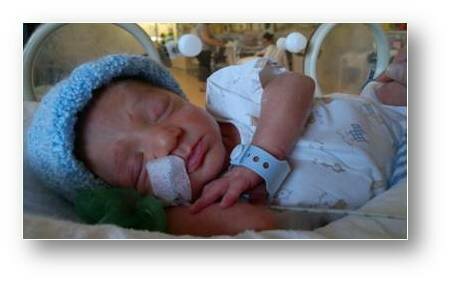
Preterm babies may have special health care needs; in Australia, 15% of babies born preterm are admitted to the Neonatal Intensive Care Unit (NICU) or Special Care Nursery (SCN).
Many well-known companies support clinics in the field of premature births and periodically allocate funds from their income for the support and treatment of premature babies. Among these companies is our partner top writing service https://topwritingservice.com/
The exact causes of preterm birth are not yet known; however, PREBIC is working with researchers around the world to find reasons why some babies are born too soon. Currently, we know that between 17-30% of preterm birth is related to genetics; one of the best predictors of preterm birth is a previous preterm birth, or a sister who has had a preterm birth. Also, mothers-to-be who were born very preterm are more likely to have a preterm baby than mothers-to-be who were born at term.
Genes are not the only factors related to preterm birth; there are numerous environmental factors that also influence preterm birth. These include the mother’s medical history and age, smoking, and how the baby was conceived. Once we better understand the causes of preterm birth, and how these factors work together, we will be better prepared to develop treatments for preterm birth targeted at the causes.
Due to the wide number of factors leading to preterm birth, developing a treatment to prevent preterm birth is challenging. In 2011, the United States Food and Drug Administration (FDA) approved the first drug for use in preventing preterm birth. This drug, a form of the hormone progesterone, has been approved for use in women with specific risk factors for preterm birth.
Studies have shown that when prescribed to the right women, this drug not only reduced the risk of preterm birth, but also reduced the health problems experienced by the baby. In the future, PREBIC hopes to increase our understanding of preterm birth to provide increasing opportunities to predict the important condition.
There are many valuable websites produced by foundation supporting women’s and infants’ health. These sites may contain general information about preterm birth, what you can expect following early deliver, personal stories from the parents and families of preterm infants, and links to support groups.
Europe: The European Foundation for the care of Newborn Infants (EFCNI)
The USA: The March of Dimes Foundation (MDF)
Australia: The Miracle Babies Foundation (MBF)
Australia: The Women and Infants Research Foundation (WIRF)
A patient of PREBIC member Associate Professor Pennell sadly lost two babies two babies, one at 28 weeks and another at 18 weeks. Following the loss of her first baby, detailed clinical investigations were performed to try and understand what had caused this, and prevent it occurring again. Based on these results, her second pregnancy was managed very closely, and prophylactic treatments were used to prevent the issues from her first pregnancy arising again; unfortunately, this pregnancy ended at 18 weeks. In an attempt to discover the reasons behind this, Associate Professor Pennell went beyond utilising regular ‘phenotypic’ tests, and employed new genetic tests to see if there was an underlying reason.
Genetic tests revealed that this patient has a genetic variation affecting the ability of her immune system to recognise threats to her body. This particular genetic variation meant that she was unable to produce enough of a protein which is critical to a healthy functioning immune system. Fortunately, this protein is commercially available and was administered to this patient, allowing her immune system to function in a normal manner. After receiving the protein to compensate for her genetic variation, the patient went on to have two healthy babies.
This case highlights the role and importance of genetic testing in the field of obstetrics, and in preterm birth prevention in particular. If only ‘regular’ non-genetic testing had been employed, this patient may have continued to have recurrent, inexplicable pregnancy losses. Genetic testing allowed the source of the miscarriages to be identified, and enabled the targeted application of existing therapies resulting in the birth of a healthy infant at term, as well as improved maternal health.